+90 533 813 89 77
info@bookingforhealth.com
What are the Functions of the Pancreas?
The pancreas is a glandular organ located in the abdomen, behind the stomach. It has both exocrine and endocrine functions. The exocrine function is to produce enzymes that aid in the digestion of food in the small intestine. The endocrine function is to produce hormones, including insulin and glucagon, which regulate glucose metabolism and help maintain proper blood sugar levels. Pancreatitis is a condition characterized by inflammation of the pancreas.
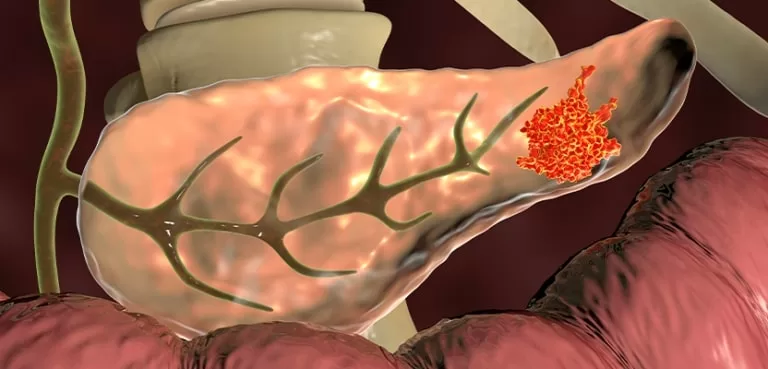
What Are the Causes and Symptoms of Pancreatic Cancer?
Pancreatic cancer, also known as pancreatic adenocarcinoma, is a type of cancer that develops in the pancreas. Certain factors increase the risk of pancreatic cancer.
The risk of pancreatic cancer increases as people get older, with most cases occurring in people over the age of 60. Smoking is a major risk factor for pancreatic cancer. People with a family history of pancreatic cancer have an increased risk of developing the disease.
People who have a history of chronic pancreatitis (inflammation of the pancreas) have a higher risk of developing pancreatic cancer.
Symptoms of pancreatic cancer; may include factors such as upper abdominal or back pain, weight loss, jaundice (yellowing of the skin and eyes), loss of appetite, nausea and vomiting, blood clots, and depression.
It’s important to note that in the early stages, pancreatic cancer may not cause any symptoms, and the symptoms that do occur are often non-specific and can be caused by other conditions. That’s why it’s important to see a doctor if you have any concerns about your health. It is also worth noting that early diagnosis and treatment are crucial for the survival rate of pancreatic cancer, which is low compared to other types of cancer.
How is Pancreatic Cancer Treated?
Treatment for pancreatic cancer typically involves a combination of surgery, chemotherapy, and radiation therapy. The specific treatment plan to be determined for pancreatic cancer depends on the stage of the cancer and the general health of the patient.
Surgery is the main treatment for pancreatic cancer that has not spread beyond the pancreas. The goal of surgery is to remove the cancerous tumor along with some surrounding healthy tissue. The most common types of surgery for pancreatic cancer are pancreaticoduodenectomy (Whipple procedure) and distal pancreatectomy. These procedures can be complex and may not be possible for some patients due to other health issues.
Targeted therapy is a new type of cancer treatment that uses medicaments to target specific molecules (such as proteins) on the surface of cancer cells that help them grow and divide. Targeted therapy is used to treat some types of pancreatic cancer, and it is often used in combination with chemotherapy.
Palliative care is a type of care that focuses on providing relief from the symptoms and stress of a serious illness, like cancer. It is used to improve the quality of life for both the patient and their family. This type of care can be provided along with curative treatments and is usually continued even when treatments are no longer working.
Radiation therapy uses high-energy beams to kill cancer cells. It is often used in combination with surgery and/or chemotherapy to help destroy any remaining cancer cells and reduce the risk of the cancer coming back. Chemotherapy is the use of medicaments to kill cancer cells. It is typically used in combination with surgery and radiation therapy to help destroy any remaining cancer cells and reduce the risk of the cancer coming back.
How Does Recovery Progress after Pancreatic Cancer Treatment?
Recovery after pancreatic cancer treatment can be a long and difficult process, and the rate of recovery can vary greatly from person to person.
During the acute recovery stage, patients will likely experience pain and discomfort and will need to limit their physical activity. They may also experience other side effects of treatment such as fatigue, nausea, and skin irritation from radiation therapy. During the subacute recovery stage, patients will begin to feel stronger and may be able to return to some of their normal activities. They may also experience side effects from treatment such as fatigue, changes in taste or smell, and difficulty eating. During the chronic recovery stage, patients will continue to make progress in regaining strength, function, and independence. They may continue to experience side effects from treatment, but these will become less severe over time.